, 77°
Wind: mph,


Lung cancer is a leading cause of cancer death for men and women in Maryland, yet only 2.9% of high-risk patients are being screened for the disease.
According to the American Lung Association’s State of Lung Cancer report released in November 2023, that number is lower than the 4.5% national rate.
At the University of Maryland Baltimore Washington Medical Center (UM BWMC) in Glen Burnie, experts in lung cancer, thoracic surgery and interventional pulmonology are working to increase lung cancer screenings and ultimately help more people get diagnosed earlier, when treatment has the best chance of being effective.
The Importance of Screening Early
“Most of that mortality (with lung cancer) is coming from the advanced stages,” said Dr. Peter Olivieri, director of interventional pulmonology at UM BWMC. “Because it is completely asymptomatic when it’s stage I. By the time a patient has symptoms from lung cancer, it’s advanced. It’s not that it’s not treatable. We still have options, but their prognosis is not going to be nearly as good as it could have been if we could have detected it early and cured it.”
When it comes to screening, the earlier, the better. Under American Lung Association guidelines updated this year, people who are between the ages of 50-80 and have a 20-pack-year or longer history of smoking are eligible for screening.
“Just like you go to your primary care doctor and get checked for blood pressure, you want to make sure you get treated so it doesn’t become a problem,” said Dr. Gavin Henry, medical director at the Tate Cancer Center at UM BWMC, and physician lead for the lung cancer screening program and chair of thoracic surgery. “Lung cancer is no different. The earlier you pick it up, the sooner you can live a normal life again.”
Screening takes less than 15 minutes and involves a low-dose CT scan. No blood work or injections are involved. Most Medicare and commercial insurance plans cover screening costs for eligible individuals. After a non-invasive, low-dose CT scan, results are reviewed by a radiologist to identify if there are any spots, or nodules, on the lungs that could indicate a problem.
Expert Care in One Place
If a nodule is cancerous after a biopsy, a multidisciplinary team of oncologists, surgeons and interventional pulmonologists at UM BWMC meet to determine the best course of care. This could include minimally invasive procedures, surgical care and radiation.
All of these services are available through UM BWMC’s Lung Center and Tate Cancer Center. Since opening more than 20 years ago, the Tate Cancer Center has cared for more than 20,000 patients, with lung cancer being the second most treated type of cancer.
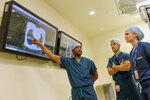
“We built a system where we are very proud that we can get patients in very quickly … review their imaging and discuss it as a team,” Olivieri said. “It’s a very interdisciplinary, team-based approach.”
Patients are seen the same week or even the same day if cancer is a possibility. Those who need surgery can take some comfort in technological advancements utilized at UM BWMC, such as state-of-the-art, minimally invasive approaches that aim to make treatment safer and help patients recover faster.
The result is a patient can get evaluated, diagnosed, staged, treated and receive follow-up all in one place.
“For them to be able to come to one place and get evaluated, diagnosed, staged, treated and ultimately follow-up afterward is what we’re able to offer, all in one location, with one integrated team, with a dedicated staff,” Olivieri said. “Not just the medical providers, but the front-office staff, as navigators, are tremendously essential for the patients. We call them navigators because they shepherd the patient through the process.”
Innovative Technology for Better Outcomes
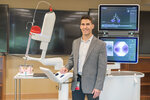
Since spring 2023, UM BWMC has had a new tool at its disposal: the ION robot, a minimally invasive technology that allows providers to sample even smaller lung nodules in harder-to-reach places in the lungs. The robotic-assisted bronchoscopy system allows health care providers to identify smaller lesions or nodules easier. It also helps physicians reach areas in the lungs that were not accessible with a traditional bronchoscopy.
“We’re trying to diagnose very small spots in the lung, and not only are they very small, but they are also moving while the patient is breathing,” Olivieri said.
The result is a more accurate diagnosis earlier, which can help patients start treatments sooner, when it’s most successful. UM BWMC’s interventional pulmonology team recently hit a milestone – surpassing 100 cases with the ION.
After the bronchoscopy, the pulmonologists do a staging — finding out if the cancer has spread and how far — so patients do not have to come back for an additional procedure.
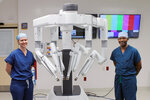
Henry has been using another robot-assisted surgical system in cases that require thoracic surgery since 2011. Called the da Vinci, the surgical system enables surgeons to perform complex and delicate procedures through small incisions.
“I have done over 1,000 robotic thoracic cases, which is quite a bit in terms of using this keyhole surgery to take out the lobe of the lung that involves the cancer, and that allows for quicker recovery of patients,” Henry said. “So, we have been able to streamline the process for improved outcomes for patients.”
Reaching Out to Understand Your Risk
In addition to educating people about screenings and offering innovative procedures and treatments, UM BWMC wants to break the stigma surrounding lung cancer.
“When you look at the other three cancers – breast, colon and prostate – most people will say they didn’t do anything in their lifestyles to get those cancers,” Henry said. “For lung cancer, people think, ‘If you didn’t smoke, it wouldn’t do this to you.’”
As many as 20% of lung cancers occur in patients who have never smoked. People who do not fit the screening profile may be able to get screened for a fee.
“Any provider can order a screening,” said Tiffany Matonak, a certified physician assistant with the thoracic surgery and lung cancer screening program. “We have a screening program that has expedited access to interventional pulmonology and thoracic, but any primary care doctor, nurse practitioner, and physician assistant can order a lung cancer screening.”
If patients have a history of smoking, they can ask their primary care doctor if they qualify for a screening. They can also take a quick online assessment to understand if they meet the criteria for a lung cancer screening at www.umbwmc.org/lunghra2.
Through early diagnosis and treatment, patients are seeing increased survival rates in Maryland. The team at UM BWMC hopes to see that trend continue as they help more patients.
“I say, ‘The best gift that you can give to me is that you have gone back to your own life and this is just a speed bump,’” Henry said. “For some patients, it’s life-changing. They are helping other people; maybe they are volunteering or being an advocate for cancer care and telling their friends. That’s what I like to see.”
For more information about UM BWMC’s pulmonary care, visit www.umbwmc.org/lung-health. To learn more about a lung screening, talk to your primary care doctor, call 410-553-8150 for an appointment, or visit www.umbwmc.org/lung-cancer-screening.
Comments
No comments on this item Please log in to comment by clicking here